
Pros & cons of continuous glucose monitoring
Continuous glucose monitoring (CGM) is an advanced way for people living with diabetes to monitor glucose levels over a period of time, in real-time. In this article, Credentialled Diabetes Educator Carolien Koreneff talks about the pros and cons of continuous glucose monitoring as well as some best practice CGM tips to ensure the health and safety of the user.
Continuous glucose monitoring overview
CGM usually consists of three parts:
- A sensor, which is a single-use plastic device with a small electrode that gets injected under the skin. Once it is inserted correctly the sensor can stay in place for six or more days, depending on the system used. The insertion does not take more than a few minutes and is essentially painless. The electrode under the skin is constantly in contact with the interstitial fluid in the body and that is how it collects glucose data.
- A transmitter, which is a device that clips onto the sensor (after this is connected on the body). The blood glucose data from the sensor is relayed to the transmitter. Which in turn, transmits the data through Bluetooth to the receiver and connected device, where you can see it in real time.
- A receiver, which can be a standalone handheld device, an app on a smart phone or an insulin pump, will automatically receive glucose levels every five minutes allowing for less finger pricks. The transmitter and receiver need to remain within 20 feet (6m) of each other so that data can be relayed without a break.
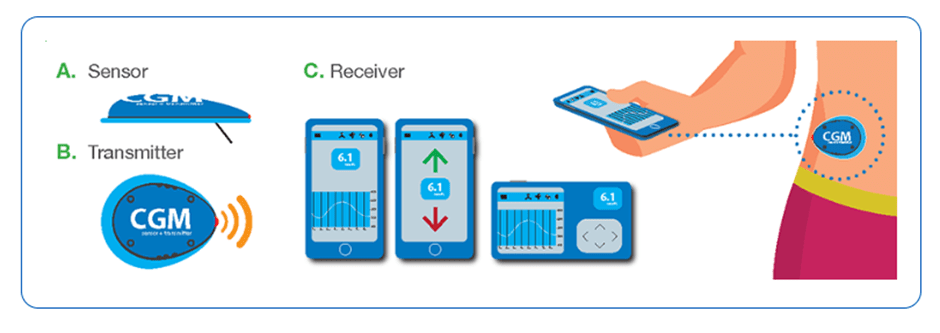
Continuous glucose monitoring devices provide information on what is happening to glucose levels every few minutes. The devices display glucose readings on a screen so the user can see, in real time, whether glucose levels are rising or falling (through trend arrows). Many devices also display graphs revealing glucose levels collected over a certain number of hours. Some systems contain an alarm to let the user know when glucose reaches high or low levels. The data collected on all devices can be uploaded to a computer for graphing and further trend analysis.
Pros of continuous glucose monitoring
Identifies trends and patterns over time
- CGM graphs can show patterns that may help identify how factors, such as food and physical activity, affect glucose levels.
- The Trend arrows show if glucose levels are stable, rising or falling and how quickly they are changing.
- CGM allows the user to see their glucose levels across the day and night, rather than just at a single point in time. For starters, this simplifies the middle-of-the-night glucose checks for parents as this allows them to remotely view the CGM data on their smartphone.
- And, CGM can help the user to understand their diabetes better, giving them more confidence in managing their diabetes and can help achieve tangible results.
Helps to reduce the risk of hypos
- CGM alarms can alert the user if they are at risk of hypoglycaemia. This allows them to act before glucose levels drop too low. Alarms can be especially useful if the user has hypo unawareness and is important for young children, who may not be able to detect their lows reliably, or may not be able to communicate their lows to parents or carers.
- Being able to see glucose levels at any time and receiving alerts if levels go outside the target range can provide peace of mind and reduce fear of hypos.
- Some CGM devices work with a compatible insulin pump and can temporarily stop insulin delivery from the pump if glucose levels drop below the target range or if the sensor predicts that the glucose level will soon become too low. This can help prevent hypos or make them easier to correct. Some CGM/pump combinations can also adjust the basal rates upwards, to deal with higher BGLs.
Ease of data sharing
- Some CGM devices allow for data sharing with others via an app on their smart device or notify them of alerts and alarms via SMS messages. This can be particularly useful for parents or carers. Remote-viewing of the data can be picked up and viewed from any other (connected) location in the world. Data can also be shared with diabetes health professionals.
Reduces the frequency of finger pricks
- Although CGM does not completely replace the need to do finger prick checks, it does reduce the number of finger pricks needed. People using CGM should speak with their diabetes health professional about when and how often they should do finger prick checks.
- CGM can be used with or without an insulin pump.
However, just slapping on a CGM won’t manage diabetes…
Cons of continuous glucose monitoring
Despite all the benefits of CGM, it has its drawbacks and there are reasons why some individuals with diabetes may choose not to add this tool, or may choose to add it intermittently to their diabetes tool kit. Even for those people for whom the benefits outweigh the drawbacks, there are important considerations to keep in mind as they use CGM. This is in order to stay safe and healthy.
CGM can be overwhelming
- Some CGM users report feeling that CGM is one more device to wear, one more thing to learn, one more set of alarms to attend to and sensor changes to remember.
- Continuous monitoring produces lots of data. Sometimes it feels like too many numbers to know what to with them. It may be useful for the user to spend the first week on CGM just watching the output without making changes; look at broad trends rather than dwelling on specific numbers; and to avoid the temptation to peek at the display too often.
Physical and emotional side-effects of CGM
- Having the CGM sensor attached to your body all the time can be annoying. Even though the sensor is not very big and most of the time other people don’t really notice it, it can leave suntan marks and sometimes cause skin irritation from the tape.
- Wearing it on the upper arm can lead to some interesting conversations with people who are curious. It can be an opportunity to educate and advocate, but if it bothers the user they could wear a long-sleeved shirt to cover the sensor or there are plenty of other areas to place the sensor where it’s less visible, like the abdomen or the buttocks.
- It may prove useful for some people to take breaks once in a while, particularly if they tend to rely on the readings and recommendations a bit too heavily.
CGM system errors and false alarms
- CGM is not fail-proof – so it’s unwise to “set it and forget it”. There can be periods when the system is “down” or the reading is not accurate. Do not rely solely on CGM alerts to detect low glucose.
- Those same alarms that are so valuable when they catch an undetected low are equally frustrating when they go off for a false low. Especially in the middle of the night. And there’s nothing more maddening than 2 hours of a display that reads only “???”. This is more common in small children and those with a lean body type. They may be more prone to sensor mix-ups, since sensors read glucose best when bathed in interstitial fluid, not when it is bumping up against muscle.
Therefore, while using CGM, it’s important to continue all the other “best practices” that keep the user safe and healthy. Remind users that symptoms of high and low glucose should not be ignored just because the CGM reading tells them that their glucose is in range. They should do regular finger prick BGLs if their sensor glucose readings do not fit with their symptoms, and to calibrate the sensor.
Best practice tips for continuous glucose monitoring
Finger pricks are still required from time to time
CGM doesn’t entirely replace finger prick blood glucose checks. Some CGM systems require a finger prick BGL to confirm the CGM reading before dosing insulin or treating a low. Some systems allow for insulin dosing and treatment of lows without a finger prick. However, finger prick BGLs are still needed for all systems when symptoms don’t match the CGM readings.
Lag time
CGM measures glucose levels in the interstitial fluid (ISF), whereas blood glucose monitors use capillary blood. There is a lag time of about 2-10 minutes between the interstitial cell fluid and the blood, which can be greater when glucose levels are rising or falling rapidly.
Lag time does not matter as much when levels are relatively consistent. However, if the glucose level has been dropping over a short period of time, a finger prick check is recommended to check for hypoglycaemia. When experiencing hypoglycaemia, users should use caution before overeating too many correction carbs. CGM can take up to one hour after hypoglycaemia to “catch up” to the actual blood glucose level.
With CGM the focus is not on the actual number, but on the trends. Knowing the speed and direction of glucose movement is much more useful than individual values.
With CGM, the focus is on the trend!
A blood glucose level of 5.5mmol/L and an arrow headed straight down is very different from being 5.5mmol/L and rising. The trend arrows are therefore useful when adjusting insulin doses up or down. For example, a rising arrow(s) indicates blood glucose is increasing and may require more insulin; a falling arrow(s) may require less insulin.
Trend arrows can also help to proactively prevent hypoglycaemia. For instance, with a glucose of 5.1mmol/L and a single arrow down, the glucose could be under 3.8mmol/L within 15-20 minutes. Taking 5-10 grams fast-acting carbs pre-emptively can help avoid the low before it even occurs.
Trend information can also help with managing diabetes around physical activity. For example, different actions are needed if the glucose level is 5.5mmol/L and steady right before exercise, compared to if it was 5.5mmol/L and rising right before exercise.
Calibration
Some CGM devices require at least two calibrations each day to improve accuracy. To calibrate, a finger prick blood sample on a blood glucose meter is used, and then entered into the receiver. A blood glucose meter reading is only valid for 12 minutes; do not wait to enter it later.
Although calibrating twice per day is essential for some CGM systems, calibrating 3-4 times per day can optimise the performance of these sensors. However, some of the newer CGM systems no longer require calibration. This is because it takes place during the manufacturing process.
To improve accuracy, it is important to take CGM calibration seriously. Do not calibrate a CGM when glucose levels are low or rapidly changing, as this can enhance inaccuracy. Be careful not to over-calibrate.
CGMs have higher inaccuracy on day one, especially in the hours after sensor insertion. Approach day one with patience and caution – especially for insulin dosing – since this is a limitation of the technology.
So, which continuous glucose monitoring system is best?
The choice of CGM device will depend on many factors, such as:
- if the person is using a compatible insulin pump,
- a smartphone or a separate receiver,
- and whether they want the option of sharing CGM readings.
Choosing the right CGM device should be done in conjunction with a diabetes health professional. They can provide all the information needed about the different types of CGM devices and answer any questions. More information on CGM is available on the National Diabetes Service Scheme (NDSS) website.
